Projekte
» Neuropathischer Schmerz

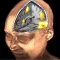
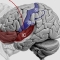
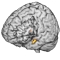
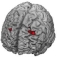
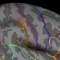
Chronic Pain changes the brain. On the functional activation level an increase in cortical excitability and an increase in cortical activation (primary sensorimotor cortex (M1/S1), anterior insula, and anterior cingulate cortex (ACC) during movement of the affected body part) could be verified especially for neuropathic pain (e.g. complex regional pain syndrome; CRPS) but also partially for other pain syndromes (e.g., craniomandibular dysfunction; CMD). For neuropathic pain this had been related to altered thalamo (Th) - cortical GABA availability. On the structural level a decrease in grey matter volume (GMV) had been demonstrated in a number of different pain syndromes (CMD, head pain, low back pain) especially in the ACC. This interacts with increased stress, increase of cigarette smoking, decreased sleeping times, increased body mass index (BMI) but inversely with the years spent with education (school, University; see glass brains on the left side of the figure). Other brain areas showing a reduction of GMV are the thalamus (for CRPS) and the anterior insula (for low back pain). On the right covariates of a population based cohort (SHIP-cohorts) for a VBM-analysis is plotted.
Most discussed contribution of our group in social media on chronic back pain and alterations of the brains grey mater volume: Fritz, H.C., McAuley, J.H., Wittfeld, K., Hegenscheid, K., Schmidt, C.O., Langner, S., Lotze, M. (2015) Chronic back pain is associated with decreased prefrontal and anterior insular gray matter. Results from a population-based cohort study.
Funding:
DFG:
- Einflussfaktoren von Gehirnveränderung bei chronischen Schmerzen LO 795/37
- Antinozizeptive Effekte und Wirkmechanismen transaurikulärer Vagusnervstimulation LO 795/38
Else Kröner Fresenius Stiftung Grundlagen des CRPS und deren Modulierbarkeit durch innovative Therapien" (S. Strauss) für 24 Monate
Domagk Stipendium für Dr. Sebastian Strauss ab 2019 für 12 Monate zur CRPS-Studie

Literatur:
Strauss S. & Lotze M. (2025) From Trauma to Chronic Pain: Mapping the Cellular Landscape of Painful Trigeminal Neuromas. Pain.
Lotze M., Strauss S. (2025) Brain Biomarkers for CRPS. Neuroscience and Biobehavioral Reviews.
Hok P., Strauss S., McAuley J., Domin M., Wang A.P., Rae C., Moseley G.L., Lotze M. (2024) Functional connectivity in complex regional pain syndrome: a bicentric study. Neuroimage.
Moseley G.L., Lotze M. (2022) Clinical and neurophysiological effects of progressive movement imagery training for pathological pain. Journal of Pain.
Domin M.*, Strauss S.*, McAuley J.H., Lotze M. (2021) Complex regional pain syndrome: thalamic GMV atrophy and associations of lower GMV with clinical and sensorimotor performance data. Journal of Pain.
Strauss S., Barby S., Härtner J., Pfannmöller J., Neumann N., Moseley G.L., Lotze M. (2021) Graded motor imagery modifies movement pain, cortical excitability and sensorimotor function in CRPS. Brain Communications.
Strauss S., Barby S., Härtner J., Neumann N., Moseley G.L., Lotze M. (2021) Modifications in fMRI representation of mental rotation following a 6 week graded motor imagery training in chronic CRPS patients. Journal of Pain.
Moseley G.L., Lotze M. (2022) Clinical and neurophysiological effects of progressive movement imagery training for pathological pain, The Journal of Pain.
Domin M.*, Strauss S.*, McAuley J.H., Lotze M. (2021) Complex regional pain syndrome: thalamic GMV atrophy and associations of lower GMV with clinical and sensorimotor performance data. Journal of Pain.
Strauss S., Barby S., Härtner J., Pfannmöller J., Neumann N., Moseley G.L., Lotze M. (2021) Graded motor imagery modifies movement pain, cortical excitability and sensorimotor function in CRPS. Brain Communications, accepted.
Strauss S., Barby S., Härtner J., Neumann N., Moseley G.L., Lotze M. (2021) Modifications in fMRI representation of mental rotation following a 6 week graded motor imagery training in chronic CRPS patients. Journal of Pain.
Kohler M., Strauss S., Horn U., Langner I., Usichenko T., Neumann N., Lotze M. (2019) Differences in neuronal representation of mental rotation in CRPS patients and healthy controls. The Journal of Pain, 20:898-907.
Jörg Pfannmöller and Martin Lotze (2018) Resting-State Biomarkers for Chronic Pain - A Network View Review in Brain and Cognition.
Usichenko T., Hacker H., Lotze M. (2017) Transcutaneous auricular vagal nerve stimulation (taVNS) might be a mechanism behind the analgesic effects of auricular acupuncture. Brain Stimulation, 10(6):1042-1044.
Landmann G, Lotze M. (2016) Neuropathische Schmerzen nach Querschnittlähmung. Neuroreha; 8: 117–121.
Lotze M. (2015) Maladaptive Plastizität bei chronisch neuropathischen Schmerzen; Der Schmerz, 30(2):127-133.
Strauß S, Grothe M, Usichenko T, Neumann N, Byblow WD, Lotze M. (2015) Inhibition of the primary sensorimotor cortex by topical anesthesia of the forearm in patients with CRPS. Pain, 156(12):2556-61.
Lotze M. and Moseley GL. (2015) Theoretical considerations for chronic pain rehabilitation. Physical Therapy, in press.
Usichenko T.I., Wesolowski T., Lotze M. (2015) Verum and sham acupuncture exert distinct cerebral activation in pain processing areas: a crossover fMRI investigation in healthy volunteers, Brain Imaging and Behavior, 9(2):236-44.
Fritz, H.C., McAuley, J.H., Wittfeld, K., Hegenscheid, K., Schmidt, C.O., Langner, S., Lotze, M. (2015) Chronic back pain is associated with decreased prefrontal and anterior insular gray matter. Results from a population-based cohort study. Journal of Pain, 17(1):111-8
Lotze, M and Di Pietro F (2014) Brain activity and reorganization in CRPS. In: The Brain Adapting with Pain: Contribution of Neuroimaging Technology to pain mechanisms. Ed: Vania Apkarian. IASP Press, in press.
DiPietro F, Stanton TR, Moseley GL, Lotze M, Mc Aulley JH (2014) Interhemispheric somatosensory differences in chronic pain reflect abnormality of the healthy side. Human Brain Mapping, in press.
Di Pietro F., Stanton, TR., Parkitny L., McAuley JH., Lotze M., Wand BW, Moseley GL (2013) Primary somatosensory cortex function in complex regional pain syndrome: a systematic review & meta-analysis. Journal of Pain, in press.
Di Pietro F., McAuley JH. Parkitny L., Lotze M., Wand BW, Moseley GL Stanton, TR., (2013) Primary motor cortex function in complex regional pain syndrome: a systematic review & meta-analysis. Journal of Pain, in press.
Walz AD., Usichenko T., Moseley GL., Lotze M. (2012) Graded motor imagery and the impact on pain processing in a case of CRPS. Journal of Clinical Pain, in press.
Friebel, U., Eickhoff, S., Lotze M. (2011) Coordinate-based meta-analysis of experi-mentally induced and chronic persistent neuropathic pain, Neuroimage, 58(4):1070-80.
Gustin S.*, Schwarz A.*, Birbaumer N., Sines N., Veit R., Larbig W., Flor H., Lotze M (2010) NMDA-antagonist and morphine decrease CRPS-pain and cerebral pain-representation. Pain, 151: 69-76.
Wesolowski T., Lotze M., Domin M., Langner S., Lehmann C., Wendt M, Usichenko T (2009) Acupuncture reveals no specific effect on primary auditory cortex - an fMRI study. NeuroReport; 20(2):116-20.
Flor H., Nikolajsen L., Jensen T.S. Phantom limb pain: a case of maladaptive CNS plasticity? Nature Neuroscience Reviews (2006) 7: 873-881.
Lotze M., Flor H., Grodd W., Larbig W., Birbaumer N. Phantom movements and pain: an fMRI study in upper limb amputees. Brain (2001) 124: 2268-2277.
Lotze M., Grodd W., Birbaumer N., Erb M., Huse E., Flor H. Does the use of a myoelectric prosthesis prevent cortical reorganization and phantom limb pain? Nature Neuroscience (1999) 2: 501-502.
Die Arbeiten wurden 2000 und 2014 mit dem Deutschen Schmerzpreis und 2002 mit dem Förderpreis der Deutschen Gesellschaft für Neurotraumatologie und Klinische Neuropsychologie ausgezeichnet